I continue to track my thyroid antibodies and I will post my results here in case this information will be useful for anyone. Trust me, I know how fluctuating thyroid hormones suck and what it means for you in terms of your mood, energy, sleep. Today is a work day and since my work place is quite formal, I should be there by 9am. Nine to five, the usual. Well I couldn’t fall asleep until 1am and woke up at 6am. I felt cold shivers and my palms were sweaty. I lay in bed for a while but it was no use, I could not fall back asleep. I did get to work slightly after 9, not very late, sat down in my cubicle, turned on my screens and stared at the code. What was I supposed to be doing today? I had forgotten. My hands continued to sweat and I had chills. Emotionally I felt as if a train had run over me. I couldn’t remember on what task I stopped at on Friday. I sensed such fatigue that I was finding it difficult to sit up straight.
Logically I knew the cause, it all happened as my endocrinologist said it would. After a period of hyperthyroidism, my TSH went to almost non-existent level and now instead of being too high, my thyroid hormones were quickly dropping. Lab test on February 1st showed that free T4 and total T3 were near their lower threshold and TSH was also low. Since TSH continues to be low, and it is the thyroid-stimulating hormone, it was not stimulating the thyroid enough to produce T3 and T4. Therefore it’s likely that today hormone levels were even lower and I went into hypothyroid state.
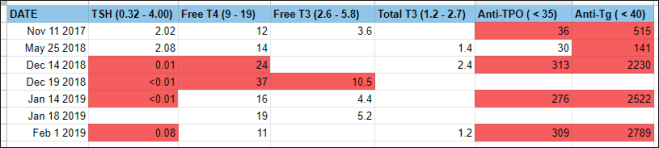
So this is what’s going on with my thyroid. I think the hypothyroidism symptoms are definitely starts as I have been getting chills, freezing even when my thermostat is at 24 degrees, not having the energy to talk to people even though I did not want to stay home on a Friday night. In theory, according to my endocrinologist, after an acute hyperthyroidism again, there will be not enough thyroid hormones stores in the thyroid gland, and therefore levels will fall. After sometime function should restore to normal, but hypothyroid state could last 8 months. I will be waiting for this normalization and in the meantime I will keep trying to reduce inflammation, because what else is there left to do.
Recently I came across a paper on green tea and exercise intervention for arthritis patients. “One-hundred and twenty subjects who had a mean age of (60.7 ± 2.53 years) and had been diagnosed with rheumatoid arthritis at least ten years previously were randomly included in this study. Patients were treated with infliximab, green tea, or a supervised exercise program for six months. Disease activity markers as well as antioxidant activity of green tea extracts were estimated before supplementation using in vitro assays. [Results] Rheumatoid arthritis patients treated with green tea for 6 months alone or in combination with infliximab or an exercise program showed significant improvement in disease activity parameters, including C-reactive protein, and erythrocyte sedimentation rate, swollen and tender joints counts, and modified Stanford Health Assessment Questionnaire score, along with an increase in serum levels of bone resorption markers, i.e., deoxypyridinoline, amino-terminal telopeptide of type 1 collagen, and bone alkaline phosphatase, at 6 months of after initial treatment. The European League Against Rheumatism and American College of Rheumatology scores revealed more clinical improvement in the disease activity of rheumatoid arthritis patients treated with green tea along with exercise compared with rheumatoid arthritis patients treated with infliximab or exercise combinations.”
I know this is just one study and we should take the results with a grain of salt, but I see no harm in including green tea and exercise in your day. I want to note that I am not looking for only ‘natural’ treatments neither am I trying to prove that they are better. I am only looking for something that I can implement. When I was referred for IV corticosteroids treatment, I was happy to receive it and did see improvements. Since then I have not been prescribed any treatment even though I did ask for it. It’s possible that something like infliximab would work for me, but I have no access to it. I have Hashimoto’s thyroiditis, celiac disease, and autoimmune encephalopathy, but inflixiamab is a medication that is prescribed for rheumatoid arthritis.
Infliximab is a monoclonal antibody that suppresses some parts of the immune system. Infliximab is a lab made molecule that binds to a specific cytokine TNF-α (chemical messenger), which is one of the causes of autoimmune reaction. TNF-α is tumor necrosis factor aplha, a cell signaling protein involved in system inflammation. Wiki states that Dysregulation of TNF production has been implicated in a variety of human diseases including Alzheimer’s disease, cancer, major depression, psoriasis and inflammatory bowel disease (IBD). Though controversial, studies of depression and IBD are currently being linked to TNF levels.
Infliximab has to be given as IV and cannot be taken orally as it would be destroyed by the digestive system. In the US the cost is about $19,000 per month and is mainly prescribed to arthritis patients who have not responded to other therapy. No one is going to prescribe it to me here in Canada.
Therefore, given that I have not been prescribed any meds at this point, and my psych and neuro keep debating whether to place me on IVIG or not, for now I have to do things on my own. Also trying green tea and exercise of course doesn’t cancel out any other treatment that I might get. I continue with helminthic therapy and hopefully I will get an IVIG trial (intravenous immunoglobulin therapy).
